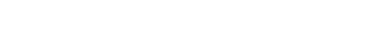
A bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.
 The medical condition known as hallux valgus is commonly referred to as a bunion. It typically occurs as a result of a misalignment in the joint of the big toe, and may cause pain and discomfort. It appears as a large bony protrusion on the side of the big toe and may be difficult to wear specific shoes. If you have a bunion, you most likely may notice tenderness and swelling around the affected joint, in addition to possible joint pain arising from the development of arthritis. This may develop at a faster rate if the bunion is not treated promptly. Some of the reasons why bunions could form may include having an abnormal foot structure such as flat feet, an inherited genetic trait, or extremely flexible ligaments and tendons. Research has shown there are different treatment techniques, which may provide moderate relief. This includes wearing shoes that fit correctly, performing gentle exercises, or wearing insoles in the shoes. It’s important to consult with a podiatrist who can determine the best treatment option for you.
The medical condition known as hallux valgus is commonly referred to as a bunion. It typically occurs as a result of a misalignment in the joint of the big toe, and may cause pain and discomfort. It appears as a large bony protrusion on the side of the big toe and may be difficult to wear specific shoes. If you have a bunion, you most likely may notice tenderness and swelling around the affected joint, in addition to possible joint pain arising from the development of arthritis. This may develop at a faster rate if the bunion is not treated promptly. Some of the reasons why bunions could form may include having an abnormal foot structure such as flat feet, an inherited genetic trait, or extremely flexible ligaments and tendons. Research has shown there are different treatment techniques, which may provide moderate relief. This includes wearing shoes that fit correctly, performing gentle exercises, or wearing insoles in the shoes. It’s important to consult with a podiatrist who can determine the best treatment option for you.
If you are suffering from bunions, contact Dr. Robert Hope of Riverside Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
If you have any questions, please feel free to contact our office located in Tuscaloosa, and Fayette, AL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
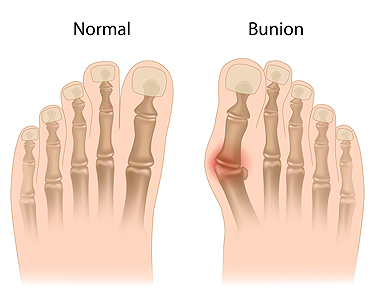
Read more about BunionsThe purpose of the body’s circulation system is to transport blood, oxygen, and nutrients throughout the body. A reduction of blood to a specific part of the body may cause one to experience symptoms of poor circulation. The most common causes of poor circulation in the feet are obesity, diabetes, and heart conditions such as peripheral artery disease (PAD). Common symptoms of poor circulation include tingling, numbness, throbbing, pain and muscle cramps.
Peripheral artery disease is a common cause of poor circulation in the legs. Symptoms of PAD are cramping, pain or tiredness in the leg or hip muscles while walking or climbing stairs. This pain tends to go away with rest and starts back up when you begin to walk. It is a condition that causes the blood vessels and arteries to become narrow. Although PAD is more common in adults over the age of 50, it may also occur in younger people. A similar condition called atherosclerosis causes arteries to stiffen up due to a buildup of plaque in the arteries and blood vessels.
Blood clots are also a common cause of poor circulation in the feet. Clots may obstruct blood vessels and if they occur in the legs, they may eventually lead to pain and discoloration. This occurrence is commonly known as deep vein thrombosis (DVT) and it may travel to the lungs. Varicose veins are another condition that may lead to poor circulation, and it is caused by incompetence of the valves in the veins. Women who are overweight are prone to developing this condition. Lastly, diabetes, which is correlated with poor blood sugar metabolism may lead to chronic poor circulation. Those with diabetes often suffer from cramping in the legs, calves, thighs and buttocks.
If you are looking for ways to avoid poor circulation there are some tips you can follow. One tip is to avoid sitting for too long. If you plan to sit down for a long period of time, you should try standing up occasionally, to improve your circulation. Another great way to avoid poor circulation is to exercise. Exercise is an excellent way to pump the heart and increase blood flow. Those who suffer from poor circulation should also avoid smoking, reduce their salt intake, and try to lose weight.
If you are experiencing symptoms from poor circulation in your feet, you should consult with your podiatrist to determine the best method for treatment for you. He or she may prescribe medication in addition to recommending specific lifestyle changes to improve your circulation.
 For people who have poor circulation, experiencing “pins and needles” and tingling are common sensations. It is not considered to be a disease, and research has shown it may be indicative of serious illnesses including heart conditions, or PAD, which is known as peripheral artery disease. When the blood circulates properly throughout the body, oxygen and essential nutrients flow easily to the organs. Poor circulation hinders the ability for this to occur. There are several symptoms that are associated with this condition, including cold feet, cramps in the muscles, lack of energy, or throbbing. History has shown that poor health habits may contribute to the onset of this ailment. These may include smoking, eating poorly, or being sedentary for long periods at a time. If you feel you have poor circulation, it’s suggested to speak with a podiatrist for possible treatment options. These may include wearing compression socks, taking prescription medicine, or surgery.
For people who have poor circulation, experiencing “pins and needles” and tingling are common sensations. It is not considered to be a disease, and research has shown it may be indicative of serious illnesses including heart conditions, or PAD, which is known as peripheral artery disease. When the blood circulates properly throughout the body, oxygen and essential nutrients flow easily to the organs. Poor circulation hinders the ability for this to occur. There are several symptoms that are associated with this condition, including cold feet, cramps in the muscles, lack of energy, or throbbing. History has shown that poor health habits may contribute to the onset of this ailment. These may include smoking, eating poorly, or being sedentary for long periods at a time. If you feel you have poor circulation, it’s suggested to speak with a podiatrist for possible treatment options. These may include wearing compression socks, taking prescription medicine, or surgery.
While poor circulation itself isn’t a condition; it is a symptom of another underlying health condition you may have. If you have any concerns with poor circulation in your feet contact Dr. Robert Hope of Riverside Podiatry. Our doctor will treat your foot needs.
Poor Circulation in the Feet
Peripheral artery disease (PAD) can potentially lead to poor circulation in the lower extremities. PAD is a condition that causes the blood vessels and arteries to narrow. In a linked condition called atherosclerosis, the arteries stiffen up due to a buildup of plaque in the arteries and blood vessels. These two conditions can cause a decrease in the amount of blood that flows to your extremities, therefore resulting in pain.
Symptoms
Some of the most common symptoms of poor circulation are:
Treatment for poor circulation often depends on the underlying condition that causes it. Methods for treatment may include insulin for diabetes, special exercise programs, surgery for varicose veins, or compression socks for swollen legs.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions, please feel free to contact our office located in Tuscaloosa, and Fayette, AL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about Causes Symptoms and Treatment for Poor Circulation in the FeetPlantar warts are growths that typically appear on the heels or other weight-bearing areas of the feet. These warts are caused by the human papillomavirus (HPV). The virus enters the body through breaks in the skin, such as cuts, that are on the bottom of the feet. Plantar warts are more likely to affect children and teenagers, people with weakened immune systems, people who have a history with plantar warts, and people who walk barefoot in environments exposed to a wart-causing virus.
If you suspect you have plantar warts, you may have the following symptoms: pain or tenderness while walking, a lesion that interrupts the ridges in the skin of your foot, small fleshy lesions on the bottom of the foot, or a callus where a wart has grown inward over a well-defined spot on the skin.
HPV causes plantar warts to form and is very common. There are more than 100 kinds of the virus in existence. However, only a few of them cause warts on the feet. The other types of HPV are likely to cause warts on other parts of the body.
If you have plantar warts, your podiatrist may try different treatment methods depending on your specific case. Some treatments for plantar warts are peeling medicines (salicylic acid), freezing medicines (cryotherapy), or surgical procedures. Laser treatments and vaccines are also used to treat plantar warts.
 The majority of warts can be unsightly and painful, and a plantar wart is no exception. This type of wart develops on the heel of the foot and will grow inward as a result of the pressure the feet endures on a daily basis. It is known to be caused by the human papillomavirus, which is also referred to as HPV, and may be more prevalent in children and people who have compromised immune systems. This contagious virus can be transmitted by direct contact with a person who may carry the germ or from an object that may have been contaminated. Some of the symptoms that might be associated with plantar warts may include a small area that may be rough in texture on the heel of the foot. Additionally, there may be tiny black dots in the center of the wart, and you may experience pain while walking or standing. If you are afflicted with plantar warts, it’s suggested to speak with a podiatrist who can offer correct treatment options that may include removal of the wart.
The majority of warts can be unsightly and painful, and a plantar wart is no exception. This type of wart develops on the heel of the foot and will grow inward as a result of the pressure the feet endures on a daily basis. It is known to be caused by the human papillomavirus, which is also referred to as HPV, and may be more prevalent in children and people who have compromised immune systems. This contagious virus can be transmitted by direct contact with a person who may carry the germ or from an object that may have been contaminated. Some of the symptoms that might be associated with plantar warts may include a small area that may be rough in texture on the heel of the foot. Additionally, there may be tiny black dots in the center of the wart, and you may experience pain while walking or standing. If you are afflicted with plantar warts, it’s suggested to speak with a podiatrist who can offer correct treatment options that may include removal of the wart.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Dr. Robert Hope from Riverside Podiatry. Our doctor will assist you with all of your foot needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
Treatment
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our office located in Tuscaloosa, and Fayette, AL . We offer the newest diagnostic and treatment technologies for all your foot needs.
Read more about Plantar WartsBlisters are pockets of fluid that occur under the top layer of your skin. These fluid pockets are usually filled with pus, blood, or serum. Blisters may itch or hurt and can appear as a single bubble or in clusters.
The most common types of blisters are friction blisters. This type of blister may be caused by wearing shoes that are too tight. Friction blisters can also occur on the hands. A change in temperature may also cause blisters on the feet. In the freezing air, frostbite on your toes can lead to blisters, as well as sunburn from hot weather.
The best way to treat a blister is to keep it clean and dry. Most blisters will get better on their own. Once the skin absorbs the fluid within the blister, it will flatten and eventually peel off. You should avoid popping your blister unless you podiatrist does it for you. Additional treatment options include applying an ice pack to the blister or using over-the-counter blister bandages to cover the affected area.
If your blister becomes discolored, inflamed, or worsens it is advised that you speak to your podiatrist. Blisters that are yellow, green, or purple may be infected and require immediate medical attention. Blisters that are abnormally colored may be a sign of a more serious underlying health condition such as herpes.
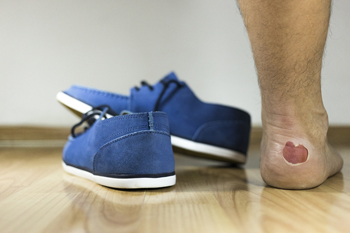 Many people are aware of the discomfort that is typically associated with blisters on the feet. A blister affects the skin on the feet, and the body’s natural response to injured skin will often result in forming a bubble of fluid over the affected area. This will protect the skin from additional damage or infection that may occur. The most common reason for blisters to develop may be wearing shoes that do not fit properly and this may cause friction as the shoes rub against the skin. Additionally, blisters may develop if you are exposed to extremely cold temperatures, which may cause frostbite to occur. Blisters may also form as a result of a harsh sunburn, or an allergic reaction to an insect bite. Treatment may generally include using a gauze covering for protection, while wearing shoes, followed by fresh air exposure when the shoes are removed, which may accelerate the healing process. It is suggested to seek the counsel of a podiatrist to learn about additional treatment options for blisters.
Many people are aware of the discomfort that is typically associated with blisters on the feet. A blister affects the skin on the feet, and the body’s natural response to injured skin will often result in forming a bubble of fluid over the affected area. This will protect the skin from additional damage or infection that may occur. The most common reason for blisters to develop may be wearing shoes that do not fit properly and this may cause friction as the shoes rub against the skin. Additionally, blisters may develop if you are exposed to extremely cold temperatures, which may cause frostbite to occur. Blisters may also form as a result of a harsh sunburn, or an allergic reaction to an insect bite. Treatment may generally include using a gauze covering for protection, while wearing shoes, followed by fresh air exposure when the shoes are removed, which may accelerate the healing process. It is suggested to seek the counsel of a podiatrist to learn about additional treatment options for blisters.
Blisters may appear as a single bubble or in a cluster. They can cause a lot of pain and may be filled with pus, blood, or watery serum. If your feet are hurting, contact Dr. Robert Hope of Riverside Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters are often the result of friction. This happens due to the constant rubbing from shoes, which can lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
Symptoms
(Blister symptoms may vary depending on what is causing them)
Prevention & Treatment
In order to prevent blisters, you should be sure to wear comfortable shoes with socks that cushion your feet and absorb sweat. Breaking a blister open may increase your chances of developing an infection. However, if your blister breaks, you should wash the area with soap and water immediately and then apply a bandage to the affected area. If your blisters cause severe pain it is important that you call your podiatrist right away.
If you have any questions, please feel free to contact our office located in Tuscaloosa, and Fayette, AL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about Blisters