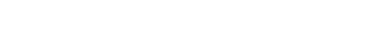
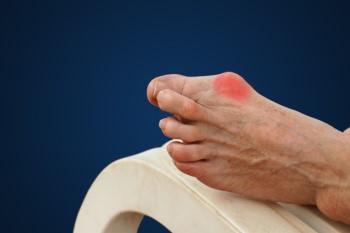
 Bunions develop due to prolonged stress on the metatarsophalangeal joint, often resulting from wearing ill-fitting shoes that force the big toe inward. This pressure causes the first metatarsal to angle outward and the big toe to point in the opposite direction, forming a noticeable bump. Additionally, genetic factors, low arches, flat feet, loose joints, and arthritis can contribute to bunion formation. Narrow, pointed-toe, or high-heeled footwear, commonly worn by women, can also heighten the risk. Furthermore, running in shoes with tapered toe boxes and elevated heels may exacerbate bunions over time. Bunions can lead to pain, discomfort, and even deformities such as hammertoes or corns. Prevention strategies include wearing wide-toed shoes, avoiding high heels, using toe spacers, and performing bunion massages to alleviate symptoms and prevent further complications. If you have a painful bunion, it is suggested that you schedule an appointment with a podiatrist for an evaluation and treatment that is best for you.
Bunions develop due to prolonged stress on the metatarsophalangeal joint, often resulting from wearing ill-fitting shoes that force the big toe inward. This pressure causes the first metatarsal to angle outward and the big toe to point in the opposite direction, forming a noticeable bump. Additionally, genetic factors, low arches, flat feet, loose joints, and arthritis can contribute to bunion formation. Narrow, pointed-toe, or high-heeled footwear, commonly worn by women, can also heighten the risk. Furthermore, running in shoes with tapered toe boxes and elevated heels may exacerbate bunions over time. Bunions can lead to pain, discomfort, and even deformities such as hammertoes or corns. Prevention strategies include wearing wide-toed shoes, avoiding high heels, using toe spacers, and performing bunion massages to alleviate symptoms and prevent further complications. If you have a painful bunion, it is suggested that you schedule an appointment with a podiatrist for an evaluation and treatment that is best for you.
If you are suffering from bunions, contact Dr. Robert Hope of Riverside Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Podiatrists often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure..
How Are Bunions Treated?
If you have any questions please feel free to contact our offices located in Tuscaloosa, and Fayette, AL. We offer the newest diagnostic and treatment technologies for all your podiatric needs.
A bunion is an enlargement of the base joint of the toe that connects to the foot, often formed from a bony growth or a patch of swollen tissues. It is caused by the inward shifting of the bones in the big toe, toward the other toes of the foot. This shift can cause a serious amount of pain and discomfort. The area around the big toe can become inflamed, red, and painful.
Bunions are most commonly formed in people who are already genetically predisposed to them or other kinds of bone displacements. Existing bunions can be worsened by wearing improperly fitting shoes. Trying to cram your feet into high heels or running or walking in a way that causes too much stress on the feet can exacerbate bunion development. High heels not only push the big toe inward, but shift one's body weight and center of gravity towards the edge of the feet and toes, expediting bone displacement.
A podiatrist knowledgeable in foot structure and biomechanics will be able to quickly diagnose bunions. Bunions must be distinguished from gout or arthritic conditions, so blood tests may be necessary. The podiatrist may order a radiological exam to provide an image of the bone structure. If the x-ray demonstrates an enlargement of the joint near the base of the toe and a shifting toward the smaller toes, this is indicative of a bunion.
Wearing wider shoes can reduce pressure on the bunion and minimize pain, and high heeled shoes should be eliminated for a period of time. This may be enough to eliminate the pain associated with bunions; however, if pain persists, anti-inflammatory drugs may be prescribed. Severe pain may require an injection of steroids near the bunion. Orthotics for shoes may be prescribed which, by altering the pressure on the foot, can be helpful in reducing pain. These do not correct the problem; but by eliminating the pain, they can provide relief.
For cases that do not respond to these methods of treatment, surgery can be done to reposition the toe. A surgeon may do this by taking out a section of bone or by rearranging the ligaments and tendons in the toe to help keep it properly aligned. It may be necessary even after surgery to wear more comfortable shoes that avoid placing pressure on the toe, as the big toe may move back to its former orientation toward the smaller toes.
 Diagnosing plantar fasciitis, an inflammatory condition in the foot which causes heel pain, involves an examination from a podiatrist. A podiatrist may first discuss medical history and symptoms with the patient. They then will perform a physical examination of the feet, checking for signs such as tenderness in the heel and arch areas. They also check for flat feet, high arches, foot swelling, and tight Achilles tendons. The podiatrist may also order X-rays or ultrasounds to rule out other potential causes of heel pain. Additionally, during the examination, the podiatrist may assess the range of motion and gait for a comprehensive understanding of the foot mechanics. This combination of methods helps the podiatrist diagnose plantar fasciitis and tailor an effective treatment plan to alleviate pain and promote healing. For an accurate diagnosis and successful management of plantar fasciitis, it is suggested that you schedule an appointment with a podiatrist.
Diagnosing plantar fasciitis, an inflammatory condition in the foot which causes heel pain, involves an examination from a podiatrist. A podiatrist may first discuss medical history and symptoms with the patient. They then will perform a physical examination of the feet, checking for signs such as tenderness in the heel and arch areas. They also check for flat feet, high arches, foot swelling, and tight Achilles tendons. The podiatrist may also order X-rays or ultrasounds to rule out other potential causes of heel pain. Additionally, during the examination, the podiatrist may assess the range of motion and gait for a comprehensive understanding of the foot mechanics. This combination of methods helps the podiatrist diagnose plantar fasciitis and tailor an effective treatment plan to alleviate pain and promote healing. For an accurate diagnosis and successful management of plantar fasciitis, it is suggested that you schedule an appointment with a podiatrist.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Robert Hope of Riverside Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
How Can It Be Treated?
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your podiatrist right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our offices located in Tuscaloosa, and Fayette, AL. We offer the newest diagnostic and treatment technologies for all your podiatric needs.
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
 Balance is a fundamental aspect of daily life, affecting activities like walking, standing, and even tying your shoes. Recent research highlights its role in overall health, with studies revealing a correlation between poor balance and increased mortality risk. Incorporating balance exercises into your routine can lower this risk and improve stability. Here are a few exercises that aim to improve balance and reduce the likelihood of falling. It’s a good idea to have a chair or wall nearby to hold on to while performing them. The first is single-leg standing, where you elevate one leg while maintaining posture and gradually increase duration. Next is heel-to-toe walking, simulating a tightrope walk to enhance balance and coordination. Finally, integrating yoga practice can help to improve body awareness and proprioception, which is needed for equilibrium. Whether you're an athlete aiming for peak performance or an older adult with balance problems, these exercises can help reduce the risk of falls and promote overall well-being. For help with foot and ankle problems related to mobility or stability, it is suggested that you visit a podiatrist for a full exam.
Balance is a fundamental aspect of daily life, affecting activities like walking, standing, and even tying your shoes. Recent research highlights its role in overall health, with studies revealing a correlation between poor balance and increased mortality risk. Incorporating balance exercises into your routine can lower this risk and improve stability. Here are a few exercises that aim to improve balance and reduce the likelihood of falling. It’s a good idea to have a chair or wall nearby to hold on to while performing them. The first is single-leg standing, where you elevate one leg while maintaining posture and gradually increase duration. Next is heel-to-toe walking, simulating a tightrope walk to enhance balance and coordination. Finally, integrating yoga practice can help to improve body awareness and proprioception, which is needed for equilibrium. Whether you're an athlete aiming for peak performance or an older adult with balance problems, these exercises can help reduce the risk of falls and promote overall well-being. For help with foot and ankle problems related to mobility or stability, it is suggested that you visit a podiatrist for a full exam.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Dr. Robert Hope of Riverside Podiatry. Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions please feel free to contact our offices located in Tuscaloosa, and Fayette, AL. We offer the newest diagnostic and treatment technologies for all your podiatric needs.
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
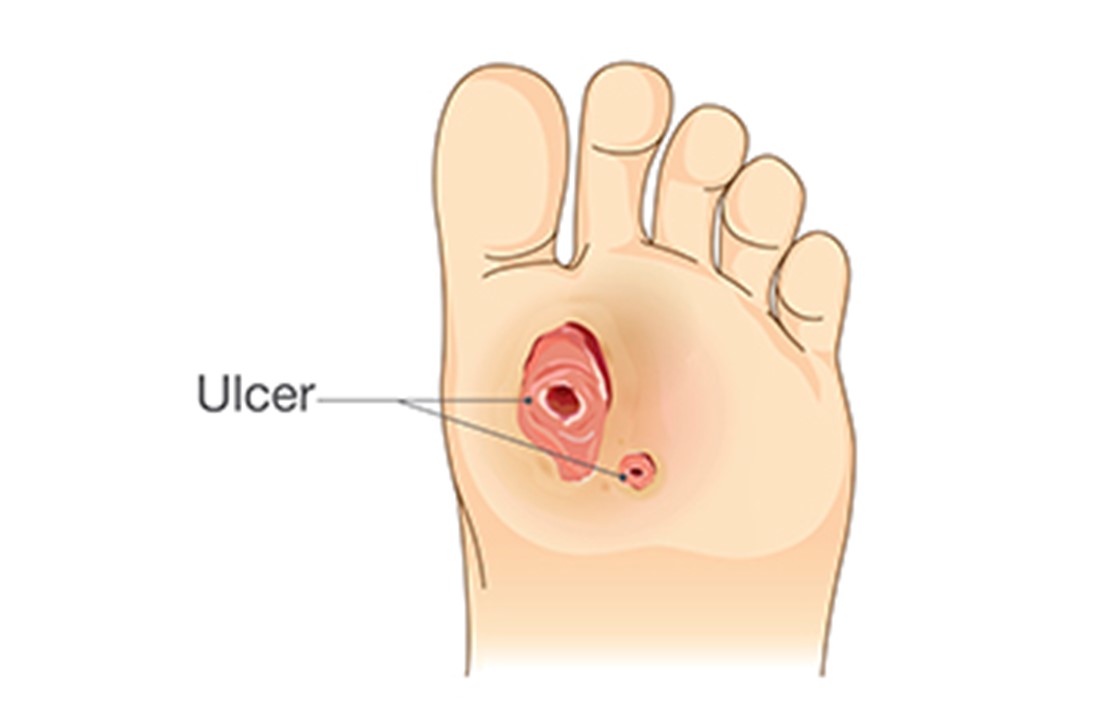 Podiatrists play a vital role in diabetic foot care, offering specialized assistance to prevent foot complications from developing. People with diabetes need to pay close attention to foot care, because high blood sugar can cause damage to nerves and result in poor blood circulation in the feet. When people cannot feel pain in their feet, they may not notice problems such as cuts and ulcers. Wounds are at even higher risk for infection as a result of poor blood flow. Podiatrists help by conducting regular foot exams to identify any issues early on. They also perform neurovascular and musculoskeletal assessments for the feet. Podiatrists educate their patients about proper foot hygiene, nail care, and daily foot checks, as well as recommend suitable footwear to prevent problems. If a patient has foot issues such as calluses, corns, or ingrown toenails, podiatrists can treat them to prevent the issues from worsening. If you have diabetes and suspect foot problems, it is suggested you consult a podiatrist who can help you manage and prevent foot-related complications due to having diabetes.
Podiatrists play a vital role in diabetic foot care, offering specialized assistance to prevent foot complications from developing. People with diabetes need to pay close attention to foot care, because high blood sugar can cause damage to nerves and result in poor blood circulation in the feet. When people cannot feel pain in their feet, they may not notice problems such as cuts and ulcers. Wounds are at even higher risk for infection as a result of poor blood flow. Podiatrists help by conducting regular foot exams to identify any issues early on. They also perform neurovascular and musculoskeletal assessments for the feet. Podiatrists educate their patients about proper foot hygiene, nail care, and daily foot checks, as well as recommend suitable footwear to prevent problems. If a patient has foot issues such as calluses, corns, or ingrown toenails, podiatrists can treat them to prevent the issues from worsening. If you have diabetes and suspect foot problems, it is suggested you consult a podiatrist who can help you manage and prevent foot-related complications due to having diabetes.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. Robert Hope of Riverside Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our offices located in Tuscaloosa, and Fayette, AL. We offer the newest diagnostic and treatment technologies for all your podiatric needs.
Diabetes affects millions of people every year. Blood vessels located all over the body are damaged due to diabetes—even the blood vessels of the feet. Neuropathy, or nerve damage, can result from slower blood flow in the legs and feet. In diabetic patients, neuropathy is very important to monitor, as diabetics are at risk for developing ulcers.
Always washing and thoroughly drying the feet are pertinent parts of diabetic foot care. There should be a focus on cleaning between the toes. Even if no pain is felt, the entire foot should be examined for redness and sores. Neuropathy can often mask the pain of sores and ulcers and can cause these conditions to be overlooked. Use a mirror to examine the underside of your feet if needed. It is recommended that diabetics wear well-fitting socks.
Patients with diabetes should have their doctor monitor their blood levels because blood sugar levels play a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised. It is very important to keep your blood sugar levels in the normal range, which can be determined by your physician. There are medications that may be prescribed to help with any neuropathy experienced by the diabetic patient. It is also advisable to visit a podiatrist if one is experiencing any conditions involving the feet, such as ingrown toenails, which in more severe cases can cause infection.
Diabetic feet must be inspected daily. Diabetic foot care at home is possible if a patient is provided with instructions from their podiatrist. Patients can relieve dry heels with creams or ointments. Suspected wounds should warrant an immediate call to the podiatrist. Gangrene is a serious problem for diabetics and can lead to sepsis and amputation in its worst cases. Early treatment and daily inspection of diabetic feet are keys to staying healthy.