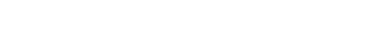
 Toenail fungus is a noticeable foot condition. A toenail that is dark and thick can be caused by a fungus that is known as dermatophytes. The nail can change shape, and the color may differ as a result of the area which is affected underneath the nail. Many times, the nail on the big toe is the first to start developing toenail fungus, and in severe cases, it may travel to other nails. There may be existing medical conditions that can lead to toenail fungus. These can include diabetes, problems with circulation, or a weakened immune system. If this condition is not treated promptly, the nails may begin to crumble, and the fungus may grow under the nail, and possibly ooze. Effective treatment may take months to completely heal the fungus, and it is important to stay consistent with applying creams, and taking medication. A podiatrist can properly diagnose and treat this condition, and it is suggested that you schedule an appointment as soon as possible so the proper treatment can begin.
Toenail fungus is a noticeable foot condition. A toenail that is dark and thick can be caused by a fungus that is known as dermatophytes. The nail can change shape, and the color may differ as a result of the area which is affected underneath the nail. Many times, the nail on the big toe is the first to start developing toenail fungus, and in severe cases, it may travel to other nails. There may be existing medical conditions that can lead to toenail fungus. These can include diabetes, problems with circulation, or a weakened immune system. If this condition is not treated promptly, the nails may begin to crumble, and the fungus may grow under the nail, and possibly ooze. Effective treatment may take months to completely heal the fungus, and it is important to stay consistent with applying creams, and taking medication. A podiatrist can properly diagnose and treat this condition, and it is suggested that you schedule an appointment as soon as possible so the proper treatment can begin.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact Dr. Robert Hope of Riverside Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Symptoms
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions please feel free to contact our offices located in Tuscaloosa, and Fayette, AL and Fayette, AL. We offer the newest diagnostic and treatment technologies for all your podiatric needs.
Fungal infection of the toenail, or onychomycosis, typically appears as a gradual change in a toenail’s texture and color that involves brittleness and darkening. The fungal infection itself occurs beneath the surface of the nail. Aside from discoloration, other symptoms include the collection of debris beneath the nail plate, white marks on the nail plate, and a foul odor emanating from the nail. If ignored, the infection can spread into other nails and the skin; in severe cases, it can hinder one’s ability to work or walk.
The toenails are particularly vulnerable to contracting infection in moist environments where people are likely to be walking barefoot, such as around swimming pools, public showers, and locker rooms. Fungal infection may also be more likely to occur in nail beds that have been injured, and sufferers of chronic diseases such as diabetes, circulatory problems, or immunodeficiency conditions are particularly prone to developing fungal nails.
Fungal nails can be primarily prevented by practicing proper hygiene and regularly examining the feet and toes. Carefully washing the feet with soap and water and thoroughly drying the feet afterwards are essential. Other tips include wearing shower shoes in public areas, changing shoes and socks daily, keeping toenails clipped at a short length, wearing breathable shoes that fit properly, wearing moisture-wicking socks, and disinfecting home pedicure tools and instruments used to cut nails.
Fungal nail treatment may vary between patients and the severity of the condition. Your podiatrist may suggest a daily routine of cleansing that spans over a period of time to ease mild infections. Over-the-counter or prescription antifungal agents may also be prescribed, including topical and/or oral medications. Debridement, or the removal of diseased nail matter and debris, may also be performed. In more severe cases, surgical treatment may be needed. In some instances, the temporary removal of the fungal nail allows for the direct application of a topical antifungal to the nail bed. In other cases, a chronically painful fungal nail that has not responded to other treatments may be permanently removed; this allows the infection to be cured and avoids the growth of a deformed nail.
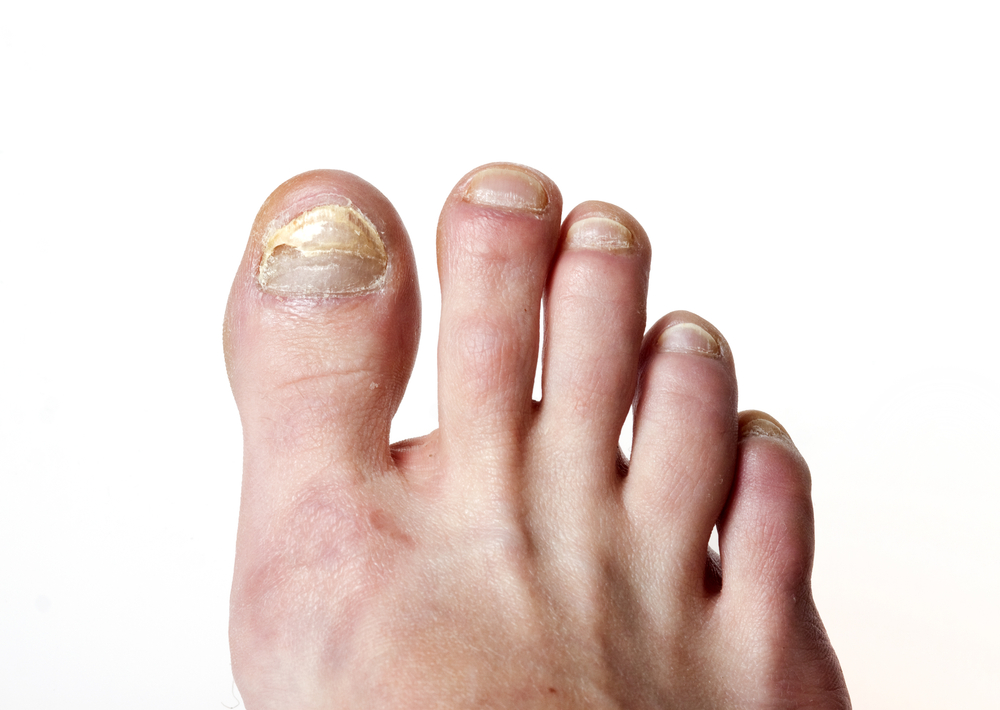
 Plantar fasciitis occurs when the connective plantar fascia tissue on the bottom of the foot becomes inflamed, or even torn, from overuse. Women, runners, people who are obese or who stand while working, are more at risk of developing plantar fasciitis. Also, having certain structural issues—such as flat feet, high arches, or tight calf muscles—can cause the plantar fascia to pull away from the heel while it is bearing weight, and may lead to this condition. Plantar fasciitis can be very painful, especially when you take your first steps in the morning, thereby engaging the plantar fascia after a long period of inactivity. Icing, stretching, anti-inflammatory medications and injections, casting, splinting, and other conservative treatments administered by a podiatrist can usually repair the plantar fascia without the need for surgery. It is suggested to make an appointment with a podiatrist to have your condition diagnosed and treated properly.
Plantar fasciitis occurs when the connective plantar fascia tissue on the bottom of the foot becomes inflamed, or even torn, from overuse. Women, runners, people who are obese or who stand while working, are more at risk of developing plantar fasciitis. Also, having certain structural issues—such as flat feet, high arches, or tight calf muscles—can cause the plantar fascia to pull away from the heel while it is bearing weight, and may lead to this condition. Plantar fasciitis can be very painful, especially when you take your first steps in the morning, thereby engaging the plantar fascia after a long period of inactivity. Icing, stretching, anti-inflammatory medications and injections, casting, splinting, and other conservative treatments administered by a podiatrist can usually repair the plantar fascia without the need for surgery. It is suggested to make an appointment with a podiatrist to have your condition diagnosed and treated properly.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Robert Hope of Riverside Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
How Can It Be Treated?
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our our offices located in Tuscaloosa, and Fayette, AL and Fayette, AL. We offer the newest diagnostic and treatment technologies for all your podiatric needs.
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
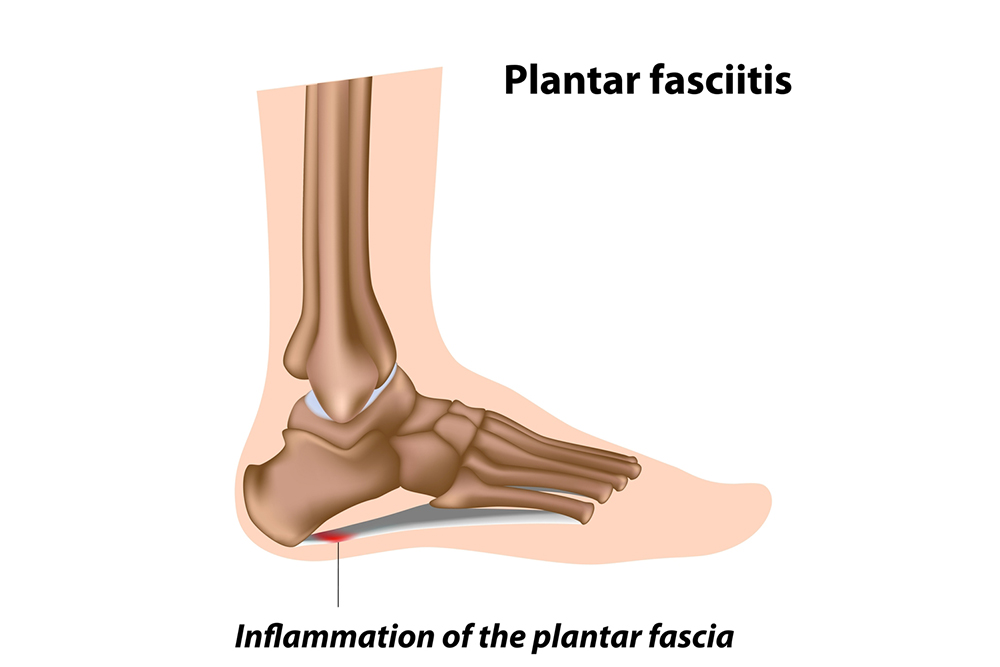
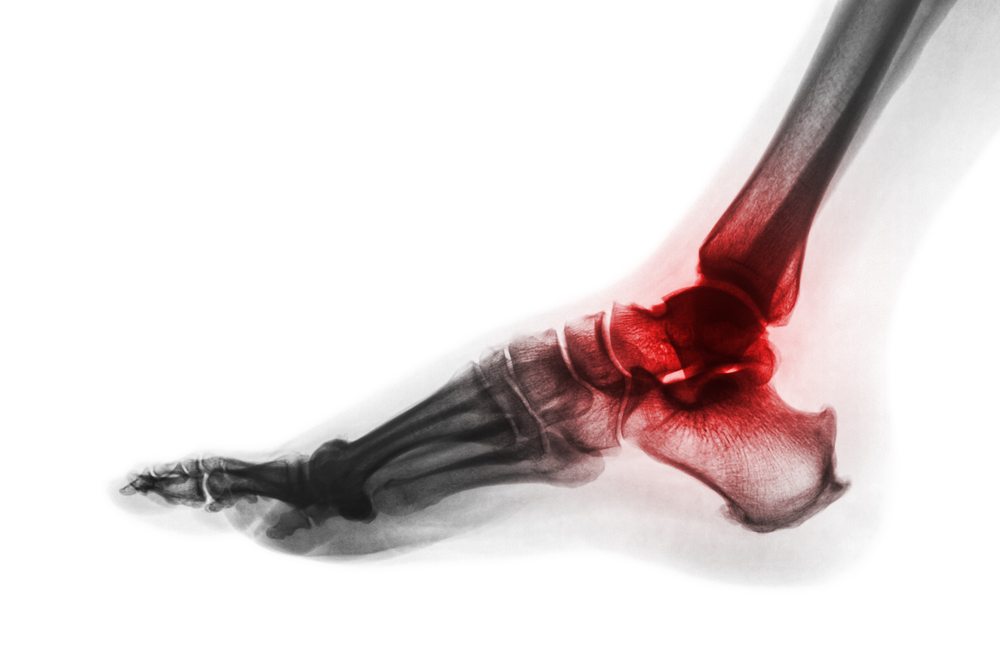 Rheumatoid arthritis can be a debilitating disease where a joint's lining (synovium) is attacked by the body’s immune system. This causes the synovium to become inflamed, which damages the surrounding tissues and ligaments. In time, this may dislocate toe joints and cause deformities such as bunions and hammertoes. Along with toe joints, rheumatoid arthritis can also occur in the ankle joint, the tarsometatarsal joints in the midfoot, and the hindfoot (heel area). While rheumatoid arthritis has no cure, a podiatrist can help treat its symptoms which, if left untreated, may inhibit a person’s ability to lead a normal life. Your podiatrist may prescribe special shoes, braces, and/or create custom orthotics to help restore functionality to the feet and relieve pain. Icing, gentle exercises, and physical therapy may also help relieve symptoms, as can corticosteroid injections. Make an appointment with a podiatrist today to begin treatment for your painful rheumatoid arthritis symptoms.
Rheumatoid arthritis can be a debilitating disease where a joint's lining (synovium) is attacked by the body’s immune system. This causes the synovium to become inflamed, which damages the surrounding tissues and ligaments. In time, this may dislocate toe joints and cause deformities such as bunions and hammertoes. Along with toe joints, rheumatoid arthritis can also occur in the ankle joint, the tarsometatarsal joints in the midfoot, and the hindfoot (heel area). While rheumatoid arthritis has no cure, a podiatrist can help treat its symptoms which, if left untreated, may inhibit a person’s ability to lead a normal life. Your podiatrist may prescribe special shoes, braces, and/or create custom orthotics to help restore functionality to the feet and relieve pain. Icing, gentle exercises, and physical therapy may also help relieve symptoms, as can corticosteroid injections. Make an appointment with a podiatrist today to begin treatment for your painful rheumatoid arthritis symptoms.
Because RA affects more than just your joints, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact Dr. Robert Hope of Riverside Podiatry. Our doctor will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact our our offices located in Tuscaloosa, and Fayette, ALand Fayette, AL. We offer the newest diagnostic and treatment technologies for all your podiatric needs.
Rheumatoid Arthritis is a chronic progressive disease that attacks several joints throughout the body. It is an autoimmune disease in which the body’s immune system mistakenly attacks the joints. As a result, the tissue inside the joints, called synovium, starts to thicken and causes pain around the joints. The synovium is responsible for creating a fluid that lubricates the joints to help them move. Approximately 1.5 million people in the United States have Rheumatoid Arthritis. Women are almost three times as likely to have RA compared to men, and it’s disease usually begins between the ages of 30 and 60. People who have a genetic history of RA are more likely to develop the disease.
Symptoms of RA may include the following sensations in the joints: pain, tenderness, swelling, redness, warmth, stiffness, and loss of range. Swollen joints are a very common symptom for those with the disease. At times, it may be minimal, but it may also be very apparent. Another typical symptom is joint stiffness. Doctors will often use the direction of morning stiffness to measure the severity of a patient’s joint inflammation. Other RA symptoms include limping, anemia, fever, and fatigue.
To diagnose RA, your podiatrist will typically request x-rays to see how much damage there is in the joints. Blood tests may also be performed to show if there are any signs of anemia, or antibodies such as the rheumatoid factor. If you have previously been diagnosed with RA, you should know the disease may spread to your feet and ankles.
There are many non-surgical options that can be used to treat this ailment. Some of these options include physical therapy, foot massages, orthotics, bracing, supportive shoes, and steroid injections. Physical therapy is useful because it will help stretch and strengthen the joints in both the foot and ankle to improve joint function. Massages can help improve blood circulation which will be good for the feet. Choosing proper footwear will allow you to walk with comfortability if you are a sufferer from RA. Lastly, bracing will help stabilize the foot joints, limit deformities and decrease pain.
In severe cases, surgery may be a treatment option that should be considered. For those who cannot walk without experiencing pain and those whose deformities can not be managed with braces, surgery should be considered. Your podiatrist will recommend surgery if he or she believes it will improve your foot biomechanics.
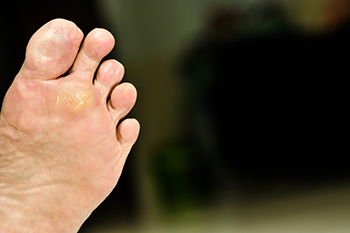 Research has shown that plantar warts affect approximately ten percent of the population. They are warts that develop on the sole of the foot, and grow inward as a result of the weight the feet endure on a daily basis. They are generally caused by the human papilloma virus (HPV), and can enter the body through small cuts in the skin on the feet. They are prone to developing on the ball and heel of the foot, and are considered to be hyperkeratotic eruptions. Plantar warts can cause severe pain and discomfort, and aggressive treatment may be necessary to relieve the pain while walking. Some patients have to alter their style of walking if they have a plantar wart, and their posture may be affected. If you have a wart on the bottom of your foot, please seek the counsel of a podiatrist who can effectively treat this condition.
Research has shown that plantar warts affect approximately ten percent of the population. They are warts that develop on the sole of the foot, and grow inward as a result of the weight the feet endure on a daily basis. They are generally caused by the human papilloma virus (HPV), and can enter the body through small cuts in the skin on the feet. They are prone to developing on the ball and heel of the foot, and are considered to be hyperkeratotic eruptions. Plantar warts can cause severe pain and discomfort, and aggressive treatment may be necessary to relieve the pain while walking. Some patients have to alter their style of walking if they have a plantar wart, and their posture may be affected. If you have a wart on the bottom of your foot, please seek the counsel of a podiatrist who can effectively treat this condition.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Dr. Robert Hope of Riverside Podiatry. Our doctor will assist you with all of your podiatric needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
Treatment
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our our offices located in Tuscaloosa, and Fayette, AL. We offer the newest diagnostic and treatment technologies for all your podiatric needs.
Plantar warts are growths that typically appear on the heels or other weight-bearing areas of the feet. These warts are caused by the human papillomavirus (HPV). The virus enters the body through breaks in the skin, such as cuts, that are on the bottom of the feet. Plantar warts are more likely to affect children and teenagers, people with weakened immune systems, people who have a history with plantar warts, and people who walk barefoot in environments exposed to a wart-causing virus.
If you suspect you have plantar warts, you may have the following symptoms: pain or tenderness while walking, a lesion that interrupts the ridges in the skin of your foot, small fleshy lesions on the bottom of the foot, or a callus where a wart has grown inward over a well-defined spot on the skin.
HPV causes plantar warts to form and is very common. There are more than 100 kinds of the virus in existence. However, only a few of them cause warts on the feet. The other types of HPV are likely to cause warts on other parts of the body.
If you have plantar warts, your podiatrist may try different treatment methods depending on your specific case. Some treatments for plantar warts are peeling medicines (salicylic acid), freezing medicines (cryotherapy), or surgical procedures. Laser treatments and vaccines are also used to treat plantar warts.